Sleep trackers display colorful charts showing REM, deep sleep, and light sleep percentages — yet most people don’t understand what these stages actually represent, why they matter for recovery, or whether the numbers their device reports are even accurate.
This guide explains the neurological and physiological changes that define each sleep stage, why your body cycles through them repeatedly each night, what happens when specific stages are disrupted, and the significant limitations of consumer sleep tracking technology.
Quick Navigation
- What Sleep Cycles Actually Are
- The Four Sleep Stages Explained
- Light Sleep: Stage 1 and Stage 2
- Deep Sleep: Stage 3 (Slow-Wave Sleep)
- REM Sleep: Rapid Eye Movement
- The 90-Minute Sleep Cycle
- Sleep Architecture Across the Night
- What Disrupts Sleep Stages
- What Sleep Trackers Actually Measure
- Sleep Stage Requirements by Age
- FAQ
What Sleep Cycles Actually Are
A sleep cycle is one complete progression through all sleep stages — light sleep, deep sleep, and REM sleep — which repeats 4-6 times per night in approximately 90-minute intervals. Your brain does not enter one sleep state and remain there all night. It cycles through different states with distinct electrical patterns, hormonal releases, and physiological functions.
Why cycles exist: Different sleep stages serve different biological functions. Deep sleep handles physical restoration and memory consolidation. REM sleep processes emotional information and strengthens neural connections. Light sleep provides transitions and maintains unconsciousness. Your body needs all stages in proper proportion for complete recovery.
According to research from the National Institutes of Health, sleep stage distribution changes across the night — early cycles contain more deep sleep, later cycles contain more REM sleep. This is why waking after 4 hours feels different than waking after 7 hours even though both represent interrupted sleep.
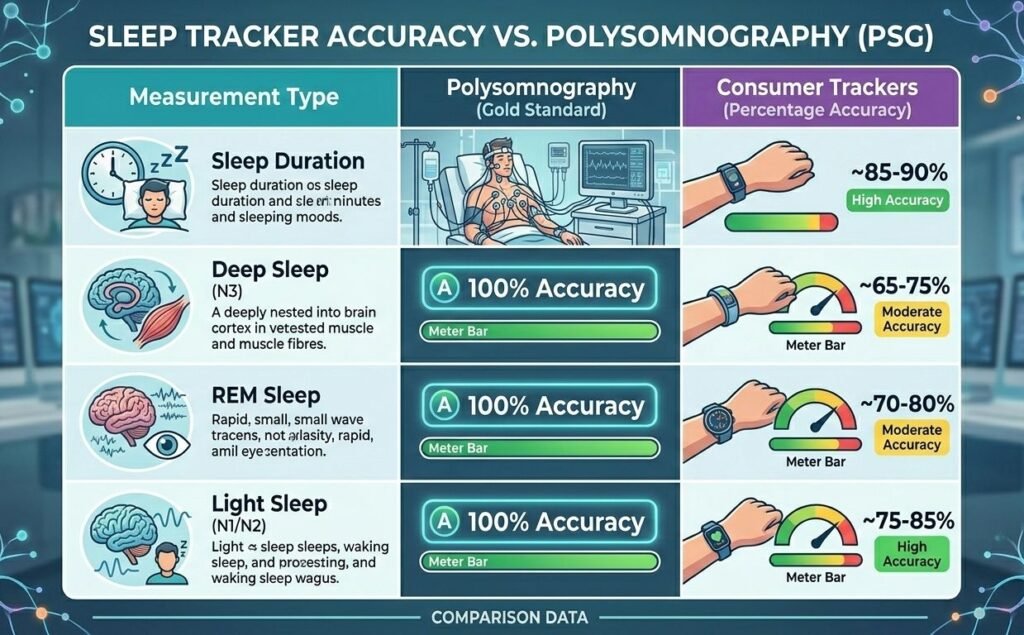
Polysomnography vs consumer trackers: Medical sleep studies use polysomnography (PSG) — electrodes measuring brain waves (EEG), eye movements (EOG), and muscle tone (EMG). Consumer sleep trackers use motion detection and heart rate — fundamentally less accurate but sufficient for general patterns.
The Four Sleep Stages Explained
Sleep consists of two major categories — Non-REM (NREM) sleep and REM sleep. NREM divides further into three stages based on brain wave patterns visible on EEG.
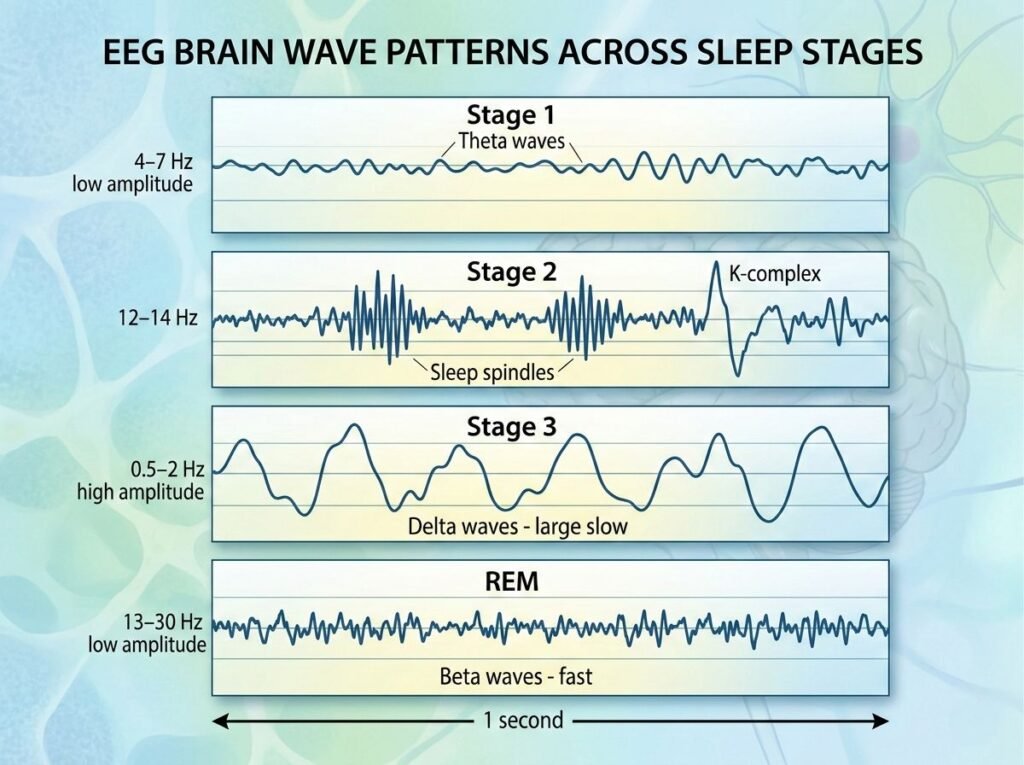
Sleep Stage Classification
Stage 1 (N1): Transition between wakefulness and sleep. Brain produces theta waves (4-7 Hz). Eyes move slowly. Muscle tone decreases. Easily awakened.
Stage 2 (N2): Light sleep where most sleep time is spent. Brain produces sleep spindles (sudden bursts of brain activity) and K-complexes (large, slow waves). Body temperature drops. Heart rate slows.
Stage 3 (N3): Deep sleep, also called slow-wave sleep (SWS). Brain produces delta waves (0.5-2 Hz) — the slowest, highest-amplitude brain waves. Difficult to wake. Sleep-walking occurs here.
REM Sleep Rapid eye movement sleep. Brain activity resembles wakefulness. Most vivid dreams occur. Muscles are temporarily paralyzed (atonia) to prevent acting out dreams.
The progression: You don’t enter deep sleep immediately. Sleep progresses from Stage 1 → Stage 2 → Stage 3 → back to Stage 2 → REM → and repeats. This cycle takes approximately 90-110 minutes and repeats 4-6 times per night.
Light Sleep: Stages 1 and 2
Light sleep comprises roughly 50-60% of total sleep time in adults — more than any other stage. Despite the name, light sleep serves critical functions.
Stage 1: Sleep Onset
Duration: 1-5 minutes per cycle (5-10 minutes total per night)
Brain activity: Theta waves (4-7 Hz) replace waking alpha waves (8-13 Hz). Brief bursts of brain activity called hypnagogic jerks may occur — the sudden muscle contractions that sometimes jolt you awake as you drift off.
Physical changes: Eye movements slow. Muscles relax but still respond to stimuli. You may experience fragmented thoughts or brief hallucinations (hearing your name called, seeing patterns).
Function: Transition stage between wake and sleep. No significant restorative function — primarily a gateway to deeper stages.
How it feels: If awakened from Stage 1, you may not realize you were asleep. This is the “dozing” feeling where you drift in and out of consciousness.
Stage 2: Core Light Sleep
Duration: 20-25 minutes in early cycles, longer in later cycles (approximately 50% of total sleep)
Brain activity: Sleep spindles (12-14 Hz bursts lasting 0.5-2 seconds) and K-complexes (large delta waves). These brain patterns are protective — sleep spindles help maintain sleep despite external noise.
Physical changes: Body temperature drops 1-2 degrees. Heart rate and breathing slow to regular rhythms. Eye movement stops. Muscles relax further.
Function: Memory consolidation — particularly procedural memory (how to do tasks) rather than declarative memory (facts and events). The brain processes and files information learned during the day. Sleep spindles correlate with intelligence and learning ability.
How it feels: Truly asleep but still somewhat responsive. Moderate noise may wake you, though sleep spindles help suppress external stimuli.
Why Stage 2 matters: Although classified as “light,” Stage 2 accounts for half your sleep and provides essential cognitive benefits. Research shows sleep spindle frequency correlates with IQ — more spindles associated with better memory consolidation and learning.
Deep Sleep: Stage 3 (Slow-Wave Sleep)
Deep sleep is the most physically restorative stage — where tissue repair, immune system strengthening, and growth hormone release occur.
Slow-Wave Sleep Characteristics
Duration: 20-40 minutes per cycle in early sleep, decreasing in later cycles (15-25% of total sleep)
Brain activity: Delta waves (0.5-2 Hz) — the slowest brain waves with highest amplitude. These large, synchronized waves reflect millions of neurons firing in unison, something only possible during deep sleep.
Physical changes: Blood pressure drops significantly. Breathing becomes slow and regular. Muscle tone minimal but present (unlike REM paralysis). Blood flow redirects from brain to muscles for physical restoration.
Hormonal release: Growth hormone secreted primarily during deep sleep. This hormone drives tissue repair, muscle growth, and cellular regeneration. Children and teenagers spend more time in deep sleep to support physical development.
Function: Physical restoration and immune system strengthening. Deep sleep is when your body repairs damaged tissues, builds bone and muscle, and strengthens immune response. Brain waste removal through the glymphatic system occurs primarily during deep sleep.
How it feels: Extremely difficult to wake. If awakened during deep sleep, you feel groggy, disoriented, confused — this is sleep inertia. May take 15-30 minutes to feel fully alert.
Why Deep Sleep Decreases with Age
Deep sleep percentage declines from approximately 20-25% in young adults to 10-15% in older adults. This is not pathological — it’s normal aging. The need for growth hormone decreases as physical development completes. Older adults still require restorative sleep but achieve it through different mechanisms.
Deep Sleep and Memory
Beyond physical restoration, deep sleep consolidates declarative memory — facts, events, knowledge learned during the day. Information transfers from temporary hippocampal storage to long-term cortical storage. This is why studying before sleep improves retention more than studying at other times.
REM Sleep: Rapid Eye Movement
REM sleep is neurologically closest to wakefulness yet paradoxically the deepest in terms of arousal threshold for some stimuli. The brain is active, but the body is paralyzed.
REM Sleep Characteristics
Duration: 10-20 minutes in early cycles, extending to 30-60 minutes in later cycles (20-25% of total sleep)
Brain activity: High-frequency, low-amplitude beta waves similar to waking state. Brain metabolism and oxygen consumption equal or exceed waking levels. This is when the most vivid, narrative dreams occur.
Physical changes: Rapid eye movements beneath closed lids (the stage’s namesake). Muscle atonia — temporary paralysis of all voluntary muscles except diaphragm and eyes. Heart rate and breathing become irregular, responding to dream content.
Why paralysis occurs: REM atonia prevents you from physically acting out dreams. Failure of this mechanism causes REM sleep behavior disorder where people physically enact their dreams — potentially dangerous.
Function: Emotional regulation and creative problem-solving. REM sleep processes emotional experiences, reducing their intensity. The brain makes novel connections between disparate information — this is why “sleeping on a problem” often produces creative solutions.
REM and Mental Health
REM sleep disruption strongly correlates with mood disorders. Depression is associated with both excessive REM (entering REM too quickly, spending too much time there) and REM fragmentation. Antidepressants often suppress REM sleep — interestingly improving mood, suggesting the relationship between REM and depression is complex.
Dreams in REM vs Non-REM
Most vivid, storylike dreams occur in REM. Non-REM dreams do occur but are typically less narrative, more thought-like, and less emotionally intense. You dream in all stages but only remember dreams if awakened directly from or shortly after REM.
Why you forget dreams: Memory consolidation during sleep applies to the day’s events, not to the dreams themselves. Dreams are typically forgotten within minutes unless you wake and consciously rehearse them.
The 90-Minute Sleep Cycle Explained
The frequently cited “90-minute sleep cycle” is an approximation. Actual cycle length varies between 80-120 minutes depending on individual physiology, age, and sleep debt.
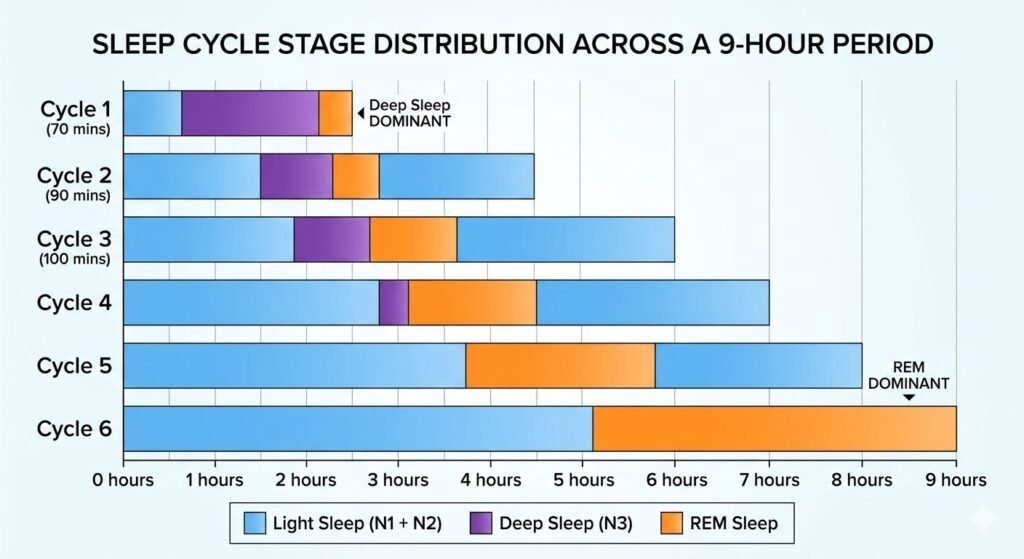
First Sleep Cycle (0-90 minutes)
Stage distribution:
- Stage 1: 5 minutes
- Stage 2: 10-25 minutes
- Stage 3 (deep sleep): 45-60 minutes
- REM: 10 minutes
First cycle contains the longest deep sleep period. Your body prioritizes physical restoration immediately after falling asleep. REM is brief — just enough to complete the cycle.
Second Sleep Cycle (90-180 minutes)
Stage distribution:
- Stage 2: 20-30 minutes
- Stage 3: 30-40 minutes
- REM: 15-20 minutes
Deep sleep decreases slightly. REM lengthens. The balance shifts toward cognitive restoration.
Third and Fourth Cycles (180-360 minutes)
Stage distribution:
- Stage 2: 25-40 minutes
- Stage 3: 10-20 minutes (may be absent in later cycles)
- REM: 25-40 minutes
Deep sleep continues decreasing. REM becomes predominant. Later cycles are primarily REM and Stage 2 oscillation. This is why waking after 6 hours prevents the longest REM periods.
Fifth and Sixth Cycles (360+ minutes)
Stage distribution:
- Stage 2: 30-50 minutes
- Stage 3: Typically absent
- REM: 30-50 minutes
Almost no deep sleep remains. Cycles consist of REM alternating with Stage 2. These final cycles contain the longest REM periods — up to 50-60 minutes of continuous REM sleep.
Why this distribution matters: Early-night sleep deprivation (going to bed late) primarily cuts deep sleep. Late-night sleep deprivation (waking early) primarily cuts REM. Both create different deficits.
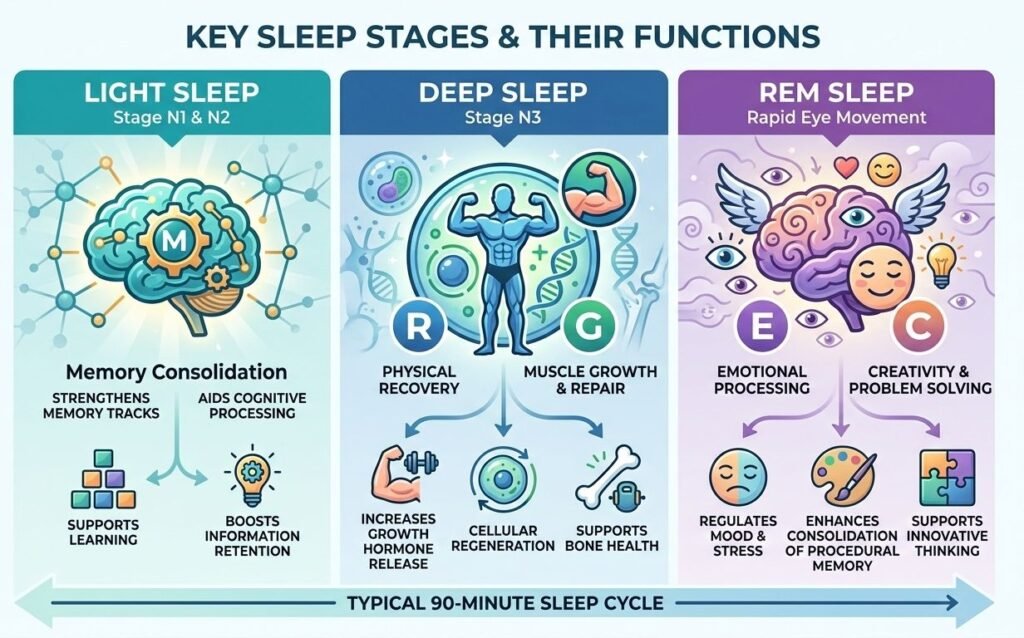
Sleep Architecture: How Stages Change Across the Night
Sleep architecture refers to the cycling pattern and proportion of stages across a full night. This architecture shifts predictably through the night and changes across the lifespan.
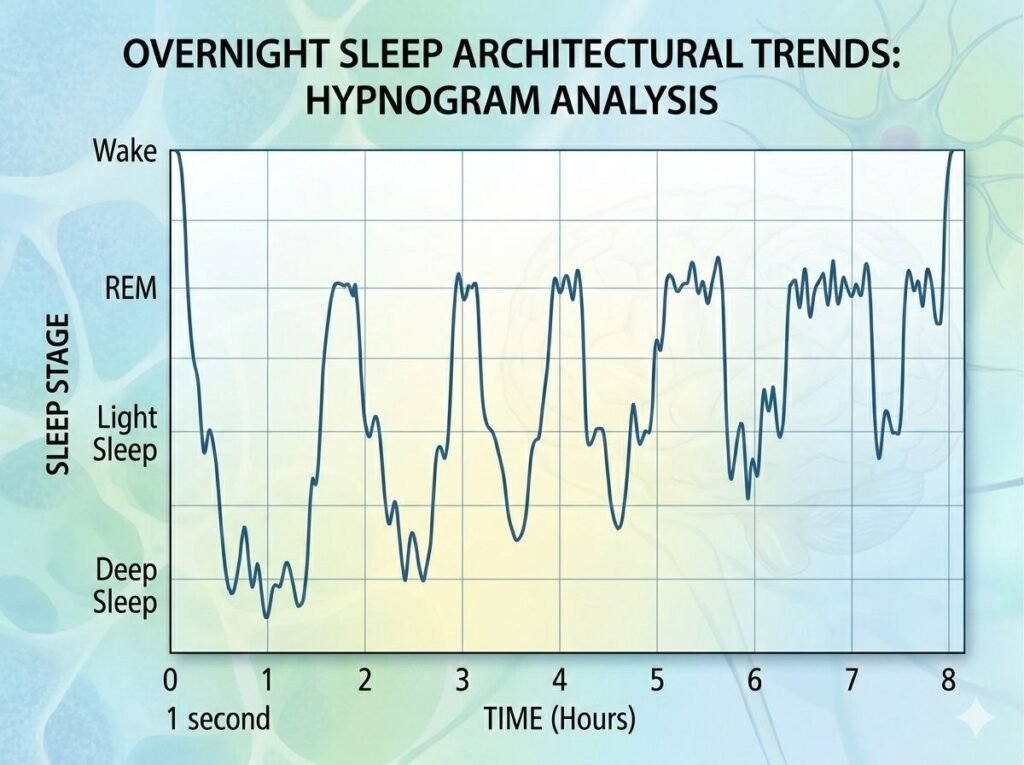
Proportion Shifts Through the Night
Hours 1-3 (Early sleep):
- Deep sleep: 60-80 minutes total
- REM: 20-30 minutes total
- Light sleep: 60-80 minutes total
Hours 3-5 (Mid sleep):
- Deep sleep: 20-40 minutes total
- REM: 40-60 minutes total
- Light sleep: 80-100 minutes total
Hours 5-7+ (Late sleep):
- Deep sleep: 0-20 minutes total
- REM: 60-100+ minutes total
- Light sleep: 60-80 minutes total
This is why alarm timing matters. Waking during REM (common in morning) versus deep sleep (rare in morning) creates different subjective experiences.
What Optimal Architecture Looks Like
Healthy adult (7-9 hours):
- Light sleep (Stage 1-2): 50-60%
- Deep sleep (Stage 3): 15-25%
- REM sleep: 20-25%
Individual variation: These percentages vary between people. Some naturally have 15% deep sleep, others 25% — both can be healthy. Consistency matters more than matching population averages.
What Disrupts Different Sleep Stages
Different factors preferentially disrupt specific sleep stages, creating distinct deficits.
Deep Sleep Disruption
Primary causes:
- Alcohol consumption (initially sedates, then fragments sleep and suppresses REM)
- Aging (natural decrease in slow-wave sleep)
- Sleep disorders (sleep apnea particularly disrupts deep sleep)
- Stress and cortisol elevation
- Evening exercise (raises core body temperature)
Effects: Reduced physical recovery, immune suppression, increased inflammation, growth hormone deficit. Deep sleep deprivation feels different than REM deprivation — more physical fatigue, increased pain sensitivity.
REM Sleep Disruption
Primary causes:
- Antidepressants (SSRIs, MAOIs suppress REM)
- Alcohol (significantly suppresses REM in first half of night)
- Sleep apnea (wakes most often during REM due to muscle relaxation)
- Irregular sleep schedule (REM is timing-dependent)
- Sleep deprivation (cuts late-night sleep when REM predominates)
Effects: Mood dysregulation, irritability, decreased creativity, impaired emotional processing. REM deprivation is subjectively more unpleasant than deep sleep deprivation.
Light Sleep Disruption
Light sleep is the most fragile — easily disrupted by noise, temperature, or light. However, because it comprises 50% of sleep, substantial light sleep still occurs even in disrupted conditions.
Primary causes:
- Environmental factors (noise, temperature, light)
- Sleep disorders (restless leg syndrome, periodic limb movement)
- Stress and hyperarousal
Effects: Less clear than deep or REM disruption. Light sleep fragmentation may indicate underlying issues but doesn’t necessarily cause specific deficits itself.
What Sleep Trackers Actually Measure
Consumer sleep trackers provide estimates of sleep stages, not medical-grade measurements. Understanding their methods and accuracy prevents over-interpreting data.
Actigraphy: Motion-Based Tracking
How it works: Accelerometers detect movement. Periods of stillness are classified as sleep. Large movements suggest wake or light sleep. Complete stillness suggests deep sleep.
Accuracy: 80-90% agreement with PSG for sleep vs wake determination. Cannot distinguish between sleep stages reliably. Most basic fitness trackers use only actigraphy.
Heart Rate Variability (HRV)
How it works: Heart rate variability increases during deep sleep and decreases during REM. Combined with motion data, HRV patterns help estimate sleep stages.
Accuracy: Moderate for deep vs REM distinction. Poor for differentiating REM from light sleep (both have low HRV). Most smartwatches and fitness trackers use HRV + actigraphy.
For detailed HRV tracking beyond sleep, see our guide on Heart Rate Variability Monitors.
Research Validation
Studies comparing consumer trackers to PSG find:
Sleep duration: High accuracy (90-95% agreement) Deep sleep: Moderate accuracy (65-75% agreement)
REM sleep: Poor to moderate accuracy (60-70% agreement) Light sleep: Calculated by subtraction (total sleep – deep – REM)
Trackers are useful for trends and relative changes (“deep sleep increased this week”) but not precise absolute measurements (“I got exactly 87 minutes of deep sleep”).
Modern sleep technology and tracking devices provide increasingly sophisticated estimates, but none match medical polysomnography accuracy.
Sleep Stage Requirements by Age
Sleep architecture changes dramatically across the lifespan. What’s normal for a child differs completely from adult or elderly sleep.
Infants (0-12 months)
Total sleep: 14-17 hours REM sleep: 50% (8+ hours) — double adult percentage Deep sleep: 25%
Light sleep: 25%
Infants spend half their sleep in REM to support rapid brain development. REM provides intense neural stimulation necessary for developing brain.
Children (3-12 years)
Total sleep: 9-12 hours REM sleep: 25-30% Deep sleep: 25-30% — highest across lifespan
Light sleep: 40-50%
Deep sleep percentage peaks in childhood to support physical growth and development. Growth hormone secretion during deep sleep drives bone and muscle growth.
Teenagers (13-18 years)
Total sleep: 8-10 hours (need), 7-8 hours (typical actual) REM sleep: 20-25% Deep sleep: 20-25% Light sleep: 50-55%
Sleep architecture similar to adults but need remains high. Chronic sleep restriction is common due to early school start times conflicting with delayed circadian rhythm.
Adults (18-64 years)
Total sleep: 7-9 hours REM sleep: 20-25%
Deep sleep: 15-25% Light sleep: 50-60%
Stable sleep architecture. Individual variation is significant — some adults function well on 7 hours, others require 9 hours. This is genetically determined.
Older Adults (65+ years)
Total sleep: 7-8 hours REM sleep: 20% Deep sleep: 10-15% — approximately half of young adult levels Light sleep: 65-70%
Deep sleep declines significantly. This is normal aging, not pathology. However, sleep becomes more fragmented — more brief awakenings, less consolidated sleep blocks.
Frequently Asked Questions
How much deep sleep do I need per night?
Adults typically need 1-2 hours (15-25% of sleep) but individual variation is significant. Some healthy adults average 50 minutes, others 120 minutes. Both can be normal. Consistency matters more than matching population averages. If you consistently get 60 minutes and feel rested, that’s likely your individual requirement.
Why do I wake up groggy even after 8 hours of sleep?
Sleep inertia — waking during deep sleep or slow-wave sleep. Your brain needs 15-30 minutes to fully transition to wakefulness. This is why alarm timing matters. Waking during light sleep or REM feels more alert than waking from deep sleep. Some alarm apps attempt to wake you during light sleep phases, though their accuracy varies.
Is it better to sleep 6 full cycles (9 hours) or wake mid-cycle at 7.5 hours?
Individual sleep need varies genetically. The “90-minute cycle” rule is an approximation that works for some people but not all. Total sleep time matters more than cycle completion. If you need 8 hours, sleeping 7.5 hours to “complete a cycle” leaves you sleep deprived. Match your biological sleep need, not theoretical cycles.
Can you make up for lost deep sleep or REM sleep?
Partially, through sleep rebound. After deep sleep deprivation, your brain increases deep sleep percentage the following nights. After REM deprivation, REM percentage increases. However, you cannot fully “make up” chronic sleep debt. Years of sleep restriction create cumulative deficits that a few long nights don’t completely resolve.
Do naps provide deep sleep and REM?
Short naps (20-30 minutes) consist primarily of light sleep. Longer naps (60-90 minutes) can include deep sleep and REM. Naps longer than 90 minutes can enter complete sleep cycles. However, napping suppresses deep sleep during the following night — the body maintains homeostatic pressure for sleep. Regular napping can indicate insufficient nighttime sleep rather than being genuinely beneficial.
Are sleep trackers accurate enough to be useful?
For trends and patterns, yes. For precise measurements, no. Trackers reliably detect total sleep time and can show relative changes (“deep sleep decreased this week”). They cannot provide medical-grade stage identification. Use trackers to identify patterns — better sleep on weekends, less REM after alcohol — not to obsess over exact percentages.
Key Takeaways
Sleep progresses through four distinct stages — two light sleep stages, one deep sleep stage, and REM sleep — cycling approximately every 90 minutes with 4-6 complete cycles per night. Each stage serves specific biological functions: light sleep (Stage 2) handles memory consolidation, deep sleep (Stage 3) provides physical restoration and immune strengthening, and REM sleep processes emotions and enables creative problem-solving.
Sleep architecture shifts predictably across the night. Early cycles prioritize deep sleep for physical recovery — 60-80 minutes total in hours 1-3. Later cycles prioritize REM sleep for cognitive and emotional processing — 60-100+ minutes total in hours 5-7. This is why going to bed late cuts deep sleep while waking early cuts REM, creating different types of deficit.
Consumer sleep trackers estimate stages using motion and heart rate variability but cannot match medical polysomnography accuracy. They’re useful for identifying trends and relative changes but not for precise stage quantification. Sleep stage requirements vary by age — children need more deep sleep for physical growth, infants need more REM for brain development, older adults naturally experience less deep sleep as growth needs decrease.
Understanding sleep stages explains why 7 hours of consolidated sleep differs from 8 hours of fragmented sleep, why alcohol helps you fall asleep but degrades sleep quality, and why waking from deep sleep feels worse than waking from light sleep. The distribution and quality of stages matters as much as total sleep duration.
Related guides:
- Complete Guide to Sleep Technology: Mattresses, Trackers & White Noise
- Heart Rate Variability Monitors: Stress Tracking Beyond Basic Fitness
- 7 Smart Health Gadgets to Track Sleep and Heart Rate
- ⭐ The 5 Best Smartwatches for Android Users Under $100 (2026)
- Best Pet Tech Gadgets: Smart Feeders, GPS Collars & Cameras for Dogs & Cats
